Explained: How to Identify Active COVID-19 Infection in People
Since the outbreak of the novel coronavirus, the ability to diagnose and test for the presence of the virus in patients has been of critical importance. However, the process and steps required in testing have not always been made clear or easy for non-experts to understand. Research!America has developed this resource to explain the scientific process behind a COVID-19 test.
During a recent Research!America alliance member call, Scott Whitaker, President and CEO of AdvaMed discussed how diagnostic companies are developing and manufacturing both “front end” tests to detect whether a person currently has COVID-19 and serology tests to determine whether someone has ever had COVID-19 by detecting the presence of antibodies. This blog explains the front end diagnostic often referred to as a “PCR” test.
COVID-19 is an RNA-based virus, meaning it does not use DNA as a genetic template like humans do. This also means when a patient is infected, cells in the body express viral RNA. In order to detect COVID-19 viral RNA, its viral genome was sequenced and used by researchers to develop a specific tool called a primer. The primer is used in one of the three critical steps described below. To increase the numbers of people tested, these steps are being optimized for use in shorter time frames, at the point-of-care, and with more efficient and accessible reagents.
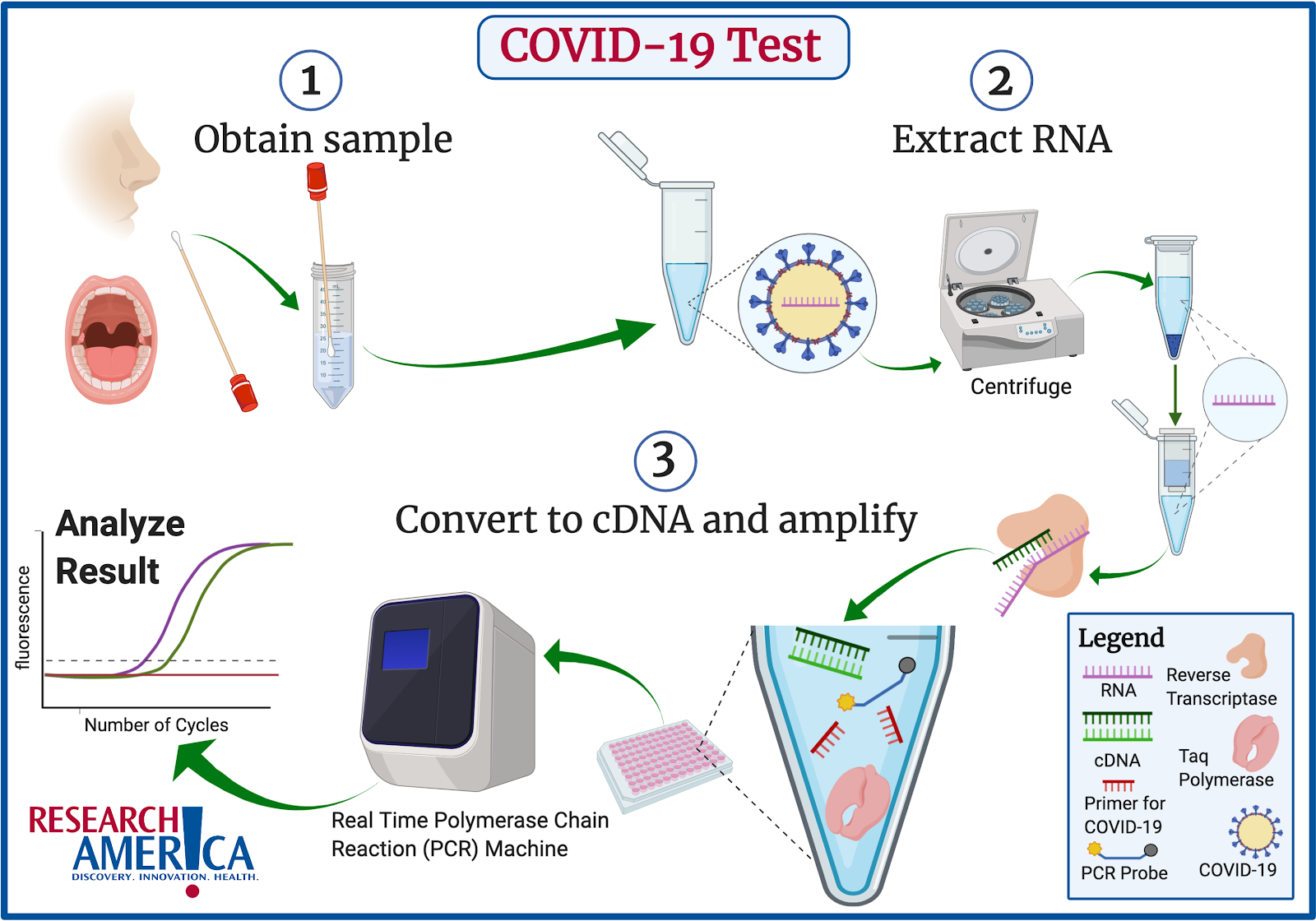
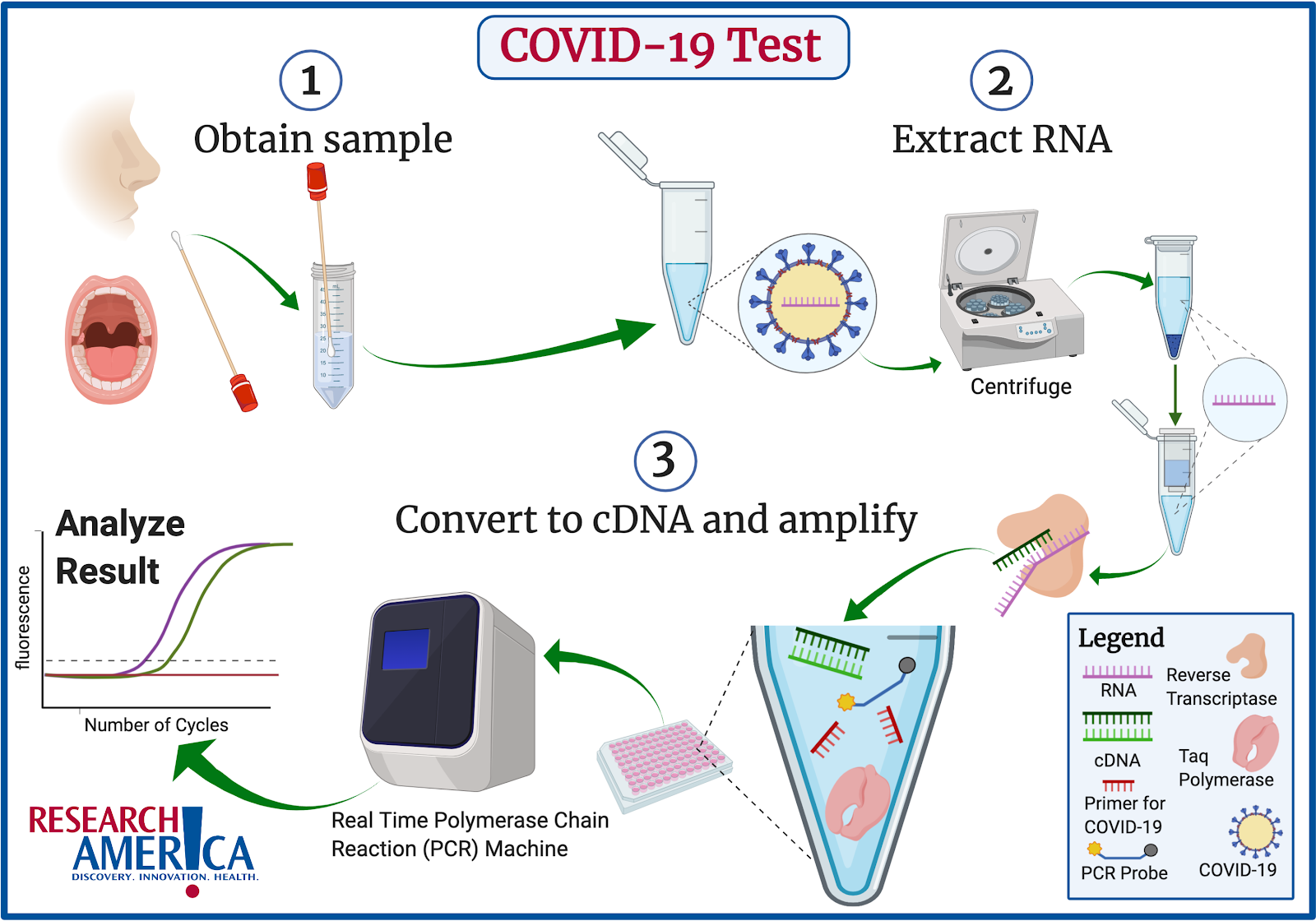
The three-step process of identifying active COVID-19 infection in a patient is depicted here:
-
The COVID-19 test starts by taking a sample from the patient’s nose or mouth. Samples are taken from these locations because they are easily accessible and are known to contain the virus.
-
The next step is to isolate RNA (pink notched line) from the patient sample. RNA is isolated because COVID-19 is an RNA based virus.
-
RNA extraction is a common laboratory procedure that can be performed with commercially available kits containing the appropriate “recipe” to separate RNA from the rest of the components in the sample.
-
A centrifuge is used to separate materials by their densities and plays an important role in the RNA extraction phase.
-
-
Once the RNA is extracted, it is converted into complementary DNA (cDNA) (green notched lines) via an enzyme called reverse transcriptase (peach-colored protein).
-
The RNA must be converted into cDNA because the final step of the test can only be performed on DNA. The cDNA is now combined with primers specific for COVID-19 (red notched line), a special enzyme called Taq polymerase (pink protein), and a special fluorescent probe (blue line with yellow and gray endings). The design of these primers enables us to specifically test for COVID-19 and they rely upon information from the sequence of the COVID-19 genome. Taq polymerase and the fluorescent probe are standard components for this test (the rapid test uses the same principle but a colorimetric rather than fluorescent probe).
-
All of these components are loaded into a plate and run in a Real Time Polymerase Chain Reaction (PCR) machine. Real Time PCR is a standard laboratory technique that amplifies a region of cDNA between the two primers. Since these primers are specific to COVID-19, the Real Time PCR test will not amplify any cDNA if the original patient sample did not contain COVID-19 RNA. If the patient sample did contain COVID-19 RNA, the amplification of the cDNA will eventually reach a level that is detected by the Real Time PCR machine using the fluorescent probe.
-
The data is then exported from the Real Time PCR machine onto a computer and analyzed. If the patient sample shows a level of COVID-19 RNA which is above the negative sample threshold and all of the controls produce the expected results, the patient tests positive for COVID-19.
-
As we wrestle to control the pandemic, accurate and accessible testing will continue to be a fundamental tool for frontline health workers, public health officials, and researchers alike. For more information on the role of testing and diagnostics in the response to COVID-19, listen to the recent Research!America alliance member call (registration required) with Scott Whitaker of AdvaMed and visit the website. Another important resource for information about the role of diagnostic tests for COVID-19 is from the American Society of Microbiology.




