The Road to Eliminating HPV-Related Cancers
“Every two minutes, one more woman dies from cervical cancer,” stressed Anna Giuliano, PhD, of the Moffitt Cancer Center. One of several speakers at the briefing “Let’s End HPV-Related Cancers” on June 27, Dr. Giuliano emphasized the severity of cervical cancer and other cancers that are linked to human papillomavirus (HPV).
This should give us pause because HPV is the most common STI – most people will be exposed at some point in their lifetime, and it has been referred to as the “common cold of STIs.” Like the common cold, HPV has different strains that have different effects on humans. At its least harmful, HPV can result in no symptoms, but at its most dangerous, it can lead to deadly cancers.
Dr. Giuliano also pointed out that HPV is an equal opportunity virus – it can infect both men and women. Though cervical cancer is the most well-known cancer caused by HPV, other HPV-related cancers affect men.
Jason Mendelsohn is one such man whose life was changed by a diagnosis of oropharyngeal – mouth and throat – cancer. He’d had no idea he could be at risk. Suddenly, Mendelsohn faced a radical tonsillectomy and neck dissection (42 lymph nodes removed from his neck), as well as chemotherapy and radiation. “My hope is that through sharing my story, other parents will be saved from having to make heart-wrenching videos to their kids saying goodbye,” said Mendelsohn.
Mendelsohn’s story is one of survival, and though many people who develop HPV-related cancers are not as lucky, the future of this field is not entirely bleak. In fact, each panelist emphasized that these cancers can actually be eliminated – “Today, the message is about prevention,” said Gilbert Omenn, MD, PhD. That’s rare to hear in the cancer field, where research is usually directed at treatments or cures rather than prevention.
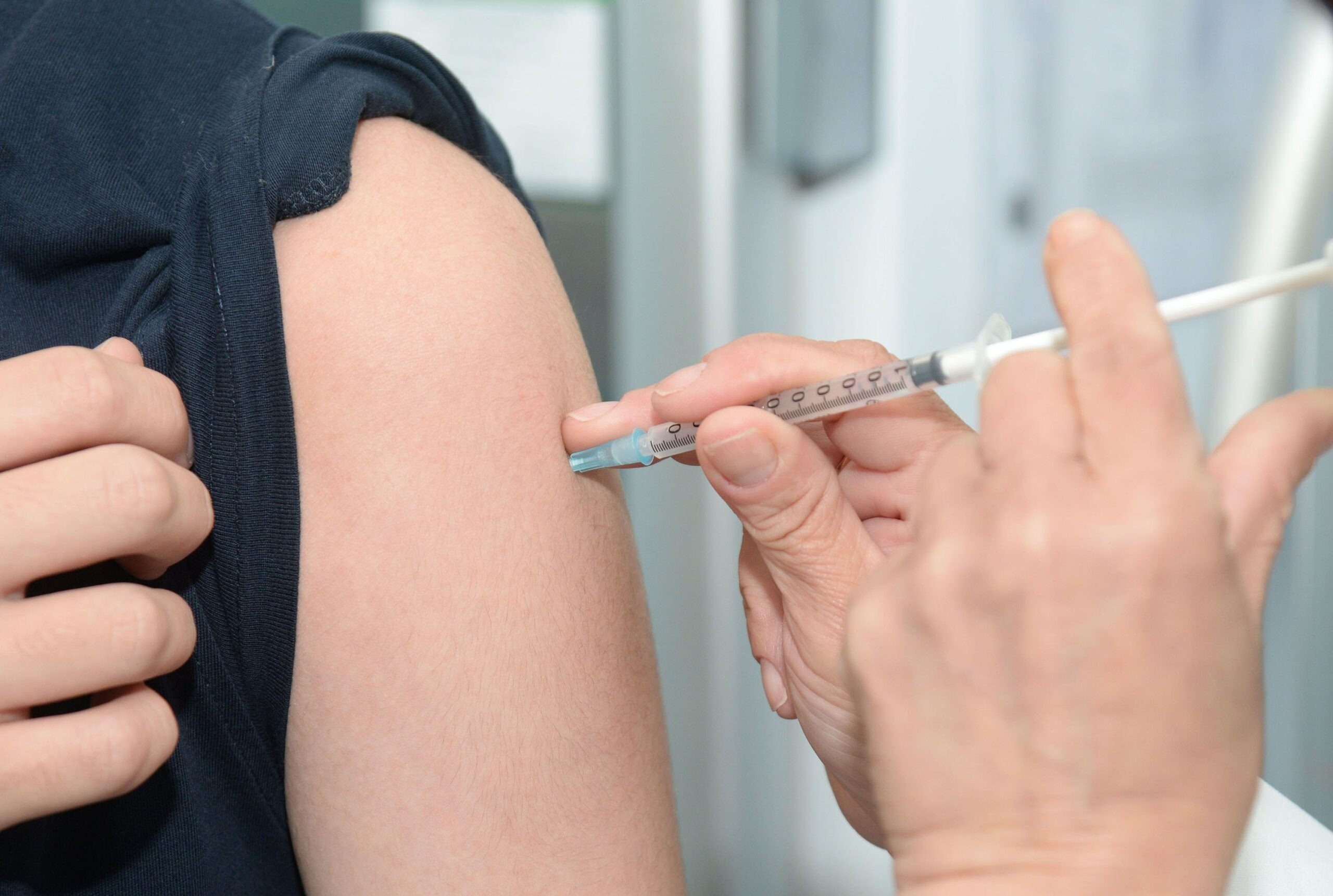
Yet by eliminating HPV, the medical community can, by extension, decrease the incidence of HPV-related cancers, and fortunately, there is an effective vaccine for HPV. The World Health Organization (WHO) currently recommends that all children ages 11 – 12 get the HPV vaccine.
Unfortunately, there is great inequity between countries, pointed out Julie Torode, PhD. Developing countries still face hurdles in distributing vaccines, as well as a looming vaccine shortage.
Even in the U.S., there are gaps in vaccination, reflecting the vaccine hesitancy often seen in highly industrialized countries surrounding concerns about safety. (Read more about a survey by the Wellcome Trust addressing public vaccine trust here.) However, all research has shown that the vaccine is safe and has no pattern of mal-effects, said John Schiller, PhD, Deputy Chief of the Laboratory of Cellular Oncology at the National Cancer Institute, who conducted research leading to the development of HPV vaccines.
Vaccination rates also vary by state, said Melinda Wharton, MD, CDC, not just due to worries about safety but also due to doctors simply not telling parents about the vaccine. Additionally, spreading information about the topic can be difficult given the taboo nature of STIs like HPV. In a video shown at the briefing, Lisa Moore, a cervical cancer patient who passed away in 2017 said, “If something like this is preventable, I don’t understand why people don’t want to prevent it. If it was a leukemia vaccine or breast cancer or prostate cancer or anything not related to sex, there’d be no question.”
Though vaccine concerns are on the forefront of the medical community’s mind, vaccination is only the first step. Screening and treatment are also key in reducing rates of HPV-related cancer. Vicki Benard, PhD, of the CDC recently conducted a study that showed that over 50% of American women with cervical cancer have not been screened, and a major reason is that they simply are not aware that they can get cervical cancer.
As with many health issues, awareness is key, and the panelists shared a sense of optimism about the prospects of combating HPV and its related cancers. Representative Kathy Castor (R-FL) is also optimistic. Said Rep. Castor, “Now we have the tools at our disposal to eliminate these cancers and save lives.”
This blog post was written by Gwendolyn Bogard, a communications intern at Research!America. The internship program is supported by the Burroughs Wellcome Fund.




