Variants Explained: The Case for Vaccinating the World

Americans across much of the U.S. might feel as if they are finally waking from a bad dream. COVID-19 cases are at their lowest levels since March 2020, vaccines are widely available, workplaces are reopening, social life has resumed, and domestic travel neared an all-time high over the July 4 holiday weekend. This “return to normal” is far from the case in many areas: countries from India to the United Kingdom to Argentina have experienced recent spikes in COVID-19 cases, with sometimes devastating results. First in India and then in the U.K., spikes in infection rates resulting in new lockdown restrictions were driven by the Delta variant – a mutation of the original SARS-CoV-2 virus. The U.S. Centers for Disease Control and Prevention lists Delta as a “variant of concern” due to it being more contagious and causing more severe infections than the original strain of SARS-CoV-2.
Delta is one of four variants currently listed as a variant of concern, and many more variants are being tracked and evaluated for risk. As the pandemic stretches on, virus variants will continue to emerge, increasing the danger of a global resurgence of COVID-19. In a connected world, prevailing over an ever-evolving, ever-changing virus cannot be achieved in isolation: victory requires a global response.
What are virus variants?
As viruses replicate, random errors can introduce DNA or RNA mutations. Most of these random mutations will be inconsequential, providing no survival or replication benefits to the virus. Some may even reduce the virus’ fitness. Every once in a while, however, a mutation may give the virus a new advantage: more contagious, longer lasting, etc. These are the variants that tend to become widespread. The most contagious variants can quickly dominate a region and cause exponential growth in caseload. For example, the B.1.1.7 variant, also known as the Alpha variant, is around 50% more transmissible than the original COVID-19 strain, allowing it to spread more quickly. The Delta variant is the fastest-spreading strain identified to date, estimated to be 40-60% more transmissible than the Alpha strain, and it has already become the dominant strain in many areas of the world, including the United States.
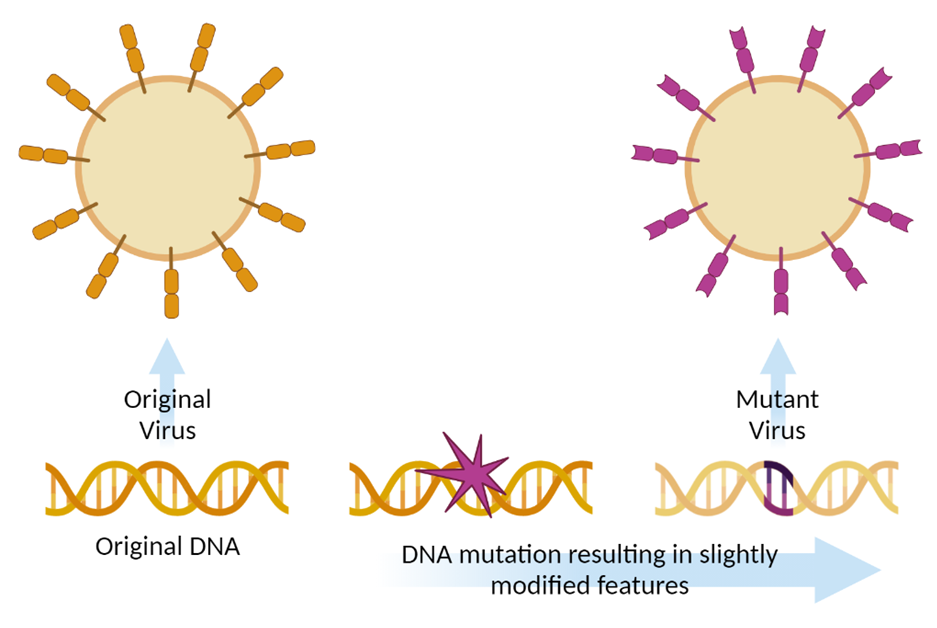
(Image created in BioRender.)
Reasons for concern
Mutations in viral variants can help the virus evade protection from vaccines or previous exposure. Vaccines work by training our immune systems to recognize and combat a particular virus shape – it’s like putting up “Wanted” posters throughout the body to make sure all defenses are ready to recognize and respond to a viral threat.
In more technical terms: antibodies generated from these immune responses recognize proteins on the surface of the virus and help direct the immune system to neutralize the threat. Viral mutations can result in changes to these surface proteins, effectively creating a disguise that makes it harder for antibodies to recognize them. Luckily, these “disguises” have so far been relatively minimal, the viral equivalent of a fake moustache. The vaccines we have now are still pretty effective at preparing the body to take on the most common SARS-CoV-2 variants.
However, this may not be the case forever. The longer a virus continues to circulate unchecked, the greater the likelihood that a mutation will produce a more effective disguise – one less like a fake moustache and more like a ski mask, rendering the virus unrecognizable to the body’s immune system. As circulating variants continue to mutate, a virus will, over time, look incrementally less like the original strain. Eventually, these variants will become different enough from the original virus that they escape detection by the immune system, and even vaccinated individuals will be susceptible to infection and illness. A good example of this is the flu virus, which mutates relatively quickly and necessitates a new vaccine each flu season.
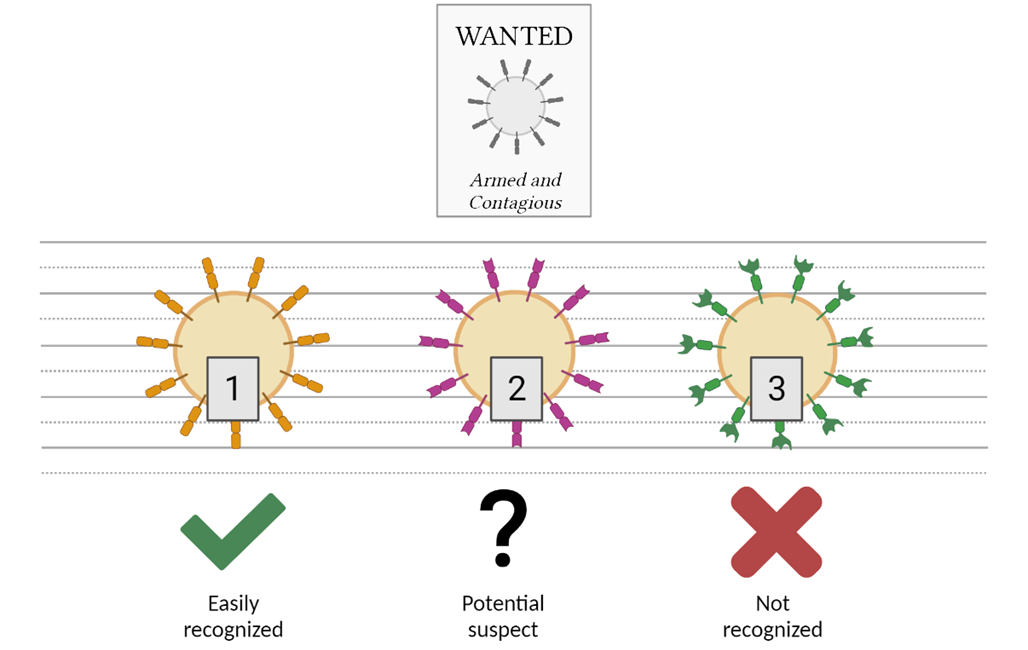
Vaccines may continue to be effective against minor variations on a virus. However, a variant that looks substantially different from the original strain may escape recognition by the immune system, potentially causing severe illness. (Image created in BioRender.)
Case for vaccination
Effective vaccination is a race between the spread and mutation rate of the virus and the speed of the public health and scientific research ecosystem to create, distribute and administer a vaccine. SARS-CoV-2 mutates relatively slowly compared to many other viruses; slow mutation of the virus and the high efficacy rates of our present vaccines has created a window of opportunity.
The best way to stop variants from emerging is to limit the chances the virus has to mutate – in other words, prevent it from spreading. This strategy of limiting spread can’t work in isolation. Some countries, like Singapore and Canada, have initiated vaccination in 65-70% of their population, putting them in reach of herd immunity. Others, like Kenya and Afghanistan, have vaccinated less than 2%. Overall, only about 25% of the world’s population has received a COVID-19 vaccine. Mutant viruses are more likely to emerge in areas with lower vaccination rates and higher rates of transmission. If and when these variants mutate in a way that allows them to evade current vaccines, the effects will be felt all around the world, even in countries with high vaccination rates.
In an era of global trade and travel, piecemeal vaccination is a failing strategy. If we want a true end to the pandemic, people in all parts of the world need access to effective vaccines, and the sooner the better. With our current distribution patterns, we risk drawing the pandemic out for years, and even nations with high vaccination rates risk resurgence and lives lost. An “us-before-them” approach makes no sense for the times – the only sensible (and indeed, the only self-preserving) course of action is to ensure that effective vaccines reach all corners of the globe.
The bad news: unequal distribution has created conditions where the virus can continue to circulate and mutate rapidly in many areas. The good news: if we hurry, we have the capacity to stop global spread of COVID-19 and curb the emergence of new variants through vaccinations. The opportunity we have requires expansive global partnerships.
This blog post was written by Jessica Scott, PhD, Research!America Science Policy Fellow.




